A Complete Guide to Dosage, Safety, and What to Expect
GLP‑1 medications are among the most talked‑about treatments today for diabetes, weight loss, and metabolic health. But a core question many people ask is:
1. How much GLP‑1 should I take?
The answer isn’t one‑size‑fits‑all. The amount depends on the specific medication, your health goals, your response, and your doctor’s guidance. In this comprehensive guide, we’ll break down dosing schedules, safety tips, practical advice, and answers to common questions.
Determining how much GLP‑1 you should take is a highly individualized process. Factors such as your health goals, current medical conditions, and tolerance to the medication all play a role. Typically, doctors start patients on a low dose and gradually increase it to minimize side effects like nausea or stomach discomfort.
Weekly injectable forms and daily oral versions follow different titration schedules, so consistency and timing are essential. Regular monitoring of blood sugar, weight, and overall well-being helps guide dose adjustments. It’s important to remember that higher doses are not always better — the optimal dose balances effectiveness with safety.
Consulting with a healthcare professional before making any changes ensures the best results. Patience is key, as the body often needs several weeks to fully adjust to GLP‑1 therapy. Ultimately, the right dose supports improved metabolic health without unnecessary risks.
2. What Are GLP‑1 Medications?
GLP‑1 stands for glucagon‑like peptide‑1, a hormone that influences appetite, blood glucose, and digestion. Medications that mimic GLP‑1 (called GLP‑1 receptor agonists) are used to help:
- Control blood sugar in type 2 diabetes
- Promote weight loss
- Reduce cardiovascular risk in some cases
These drugs work by slowing gastric emptying, increasing feelings of fullness, and improving insulin secretion.
GLP‑1 medications are a class of drugs that mimic the naturally occurring hormone glucagon-like peptide‑1 (GLP‑1) in the body. This hormone helps regulate blood sugar by stimulating insulin release when needed and slowing down the rate at which food leaves the stomach, which can reduce appetite.
As a result, GLP‑1 medications are commonly prescribed to manage type 2 diabetes and support weight loss in people with obesity. These drugs come in both injectable and oral forms, and each has a specific dosing schedule and mechanism of action. By influencing glucose metabolism and satiety signals, GLP‑1 medications can improve overall metabolic health, support long-term weight management, and reduce cardiovascular risk in some patients.
They are most effective when combined with lifestyle measures such as a balanced diet and regular physical activity.
3. Standard GLP‑1 Dosage Guidelines (by Medication)
GLP‑1 medications have specific dosage guidelines that vary depending on the drug and the treatment goal. For most patients, therapy starts at a low dosage to allow the body to adjust, then gradually increases over several weeks.
For example, semaglutide (Ozempic, Wegovy) often begins at a dosage of 0.25 mg weekly before stepping up to higher dosages, while oral forms like Rybelsus start at 3 mg daily and increase to 7–14 mg as tolerated. Liraglutide (Victoza, Saxenda) starts at a 0.6 mg dosage daily and can be titrated to 1.8–3 mg depending on whether the focus is on blood sugar control or weight management.
Other medications like tirzepatide (Mounjaro) and dulaglutide (Trulicity) also follow structured dosage schedules to optimize effectiveness and reduce side effects. Because each medication differs in strength, formulation, and frequency, following the prescribed dosage schedule and consulting your healthcare provider is essential for safe and effective treatment.
You can easily see the standard GLP‑1 dosage guidelines in the infographic below.
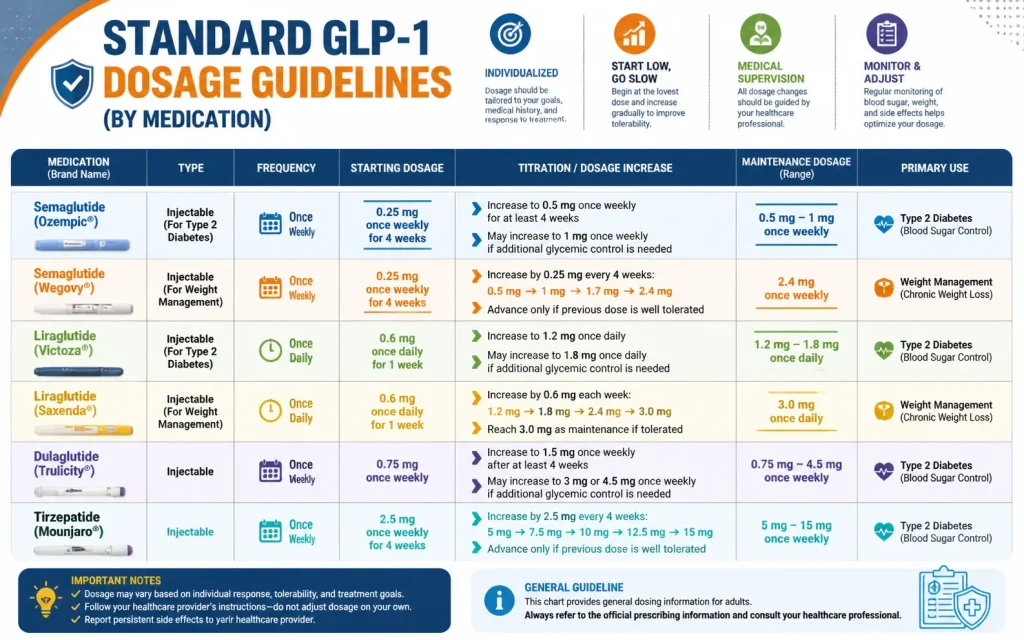
Each GLP‑1 medication has its own approved dosage schedule. These are general starting points — your doctor will tailor the dosage to your individual needs.
1. Semaglutide (Ozempic, Wegovy, Rybelsus)
Semaglutide is one of the most commonly prescribed GLP‑1 medications.
Weekly Injectable (Ozempic / Wegovy):
- Start: 0.25 mg once weekly for ~4 weeks
- Next: Increase to 0.5 mg weekly
- Further Increase: Up to 1.0 mg and higher based on results
- Maximum dose for weight loss (Wegovy): 2.4 mg weekly over several weeks with step‑up titration.
Oral (Rybelsus):
- Start: 3 mg daily for ~30 days
- Therapeutic: Increase to 7 mg daily
- Max: 14 mg daily if needed.
2. Liraglutide (Victoza, Saxenda)
- Start: 0.6 mg daily
- Increase: 1.2 mg → 1.8 mg for blood sugar control
- Weight‑loss dosing (Saxenda): Titrates up to 3.0 mg daily.
3. Tirzepatide (Mounjaro / Zepbound)
This is a dual GLP‑1/GIP medication with higher dose ranges:
- Starting: 2.5 mg weekly
- Titration: Up to 15 mg weekly depending on tolerance and goals.
Other GLP‑1 Options:
- Dulaglutide (Trulicity): Typically starts around 0.75 mg weekly
- Exenatide: Twice daily or once weekly, depending on the formulation.
4. How Your Dose Is Determined?
The appropriate GLP‑1 dose is determined by several individual factors, making it a personalized decision rather than a one-size-fits-all approach. Your medical condition, such as type 2 diabetes or obesity, plays a key role in deciding the starting dose and the speed of titration.
Your body’s tolerance to the medication is also considered, as some people experience gastrointestinal side effects that require slower dose increases. Additionally, your treatment goals—whether controlling blood sugar, promoting weight loss, or reducing cardiovascular risk—affect the dosing strategy.
Healthcare providers also monitor lab results, weight changes, and overall well-being to adjust doses safely over time. By taking these factors into account, clinicians can find the optimal balance between effectiveness and minimizing side effects, ensuring the therapy works safely for your specific needs.
Dosing is not random — it’s based on several key factors:
✓ Your Condition
- Type 2 diabetes: Often requires steady doses to control glucose.
- Weight management: Gradual titration helps minimize side effects.
✓ How You Tolerate the Medication
Doctors usually start low and increase gradually to reduce nausea, vomiting, or other gastrointestinal side effects.
✓ Your Treatment Goals
Some people use GLP‑1 medicines primarily to lower A1C, while others focus on weight loss or cardiovascular risk reduction.
5. Important Principles of GLP‑1 Dosing
When it comes to GLP‑1 dosage, there are a few key principles that help ensure safety and effectiveness. First, therapy typically begins at the lowest possible dosage, allowing your body to adjust and minimizing side effects like nausea or bloating.
Gradual titration of the dosage is essential—dosages are usually increased only after several weeks at a stable level. Consistency is also critical, whether you are using a daily oral medication or a weekly injectable, as this maintains steady blood levels of the drug. Monitoring is another important principle; tracking blood sugar, weight, and overall health helps guide dosage adjustments.
Finally, all dosage changes should be made under the supervision of a healthcare professional, ensuring that the therapy is optimized for your specific needs while reducing the risk of adverse effects. Following these principles creates a structured, safe, and effective approach to GLP‑1 therapy.
Here’s a simple overview of the dosing approach many clinicians use:
✅ Start at the lowest effective dose
- This gives your body time to adjust and helps reduce side effects.
✅ Titrate slowly over weeks or months
- Most GLP‑1s are increased only after a month or so at the current dose.
✅ Stick to a regular schedule
- Weekly injectables are given on the same day each week.
- Daily oral or injectable meds should be taken at roughly the same time each day.
✅ Consult your doctor before making adjustments
- Dose changes should always be guided by a healthcare professional.
6. Tips to Manage Side Effects
Managing side effects is an important part of GLP‑1 therapy. Start by taking the medication exactly as prescribed and avoid skipping doses. Eating smaller, more frequent meals can help reduce nausea and bloating. Staying well-hydrated supports digestion and overall comfort. Avoiding very fatty or spicy foods may minimize gastrointestinal discomfort.
Introducing new doses gradually allows your body to adjust more easily. Light physical activity, like walking after meals, can aid digestion. Keep a symptom journal to track patterns and discuss them with your doctor. If side effects are persistent, consult your healthcare provider before making any changes. Sometimes, adjusting the timing of your dose can improve tolerance.
You can refer to the infographic below for practical tips to manage common side effects of GLP‑1 medications

Patience is key, as most side effects decrease over time as your body adapts.
GLP‑1 medications have known side effects, especially early in treatment. Common issues include nausea, diarrhea, or discomfort. Here’s how to manage them:
- Eat smaller meals
- Stay hydrated
- Avoid very fatty or spicy foods
- Increase the dose more slowly if needed
- Talk to your doctor about anti‑nausea options
Always communicate with your provider if side effects are severe or persistent.
Quick Takeaways
- GLP‑1 drugs mimic a hormone that affects appetite and insulin response.
- Dosing schedules vary significantly between drugs.
- Most therapies start low and increase gradually.
- Weekly injectables differ from daily products.
- Always use under medical supervision.
Safety and Precautions
GLP‑1 therapies are generally safe when prescribed appropriately. Important safety considerations include:
⚠️ History of thyroid C‑cell tumors – Certain GLP‑1 medications are contraindicated.
⚠️ Pancreatitis – Rare but serious, discontinue and seek care if intense pain occurs.
⚠️ Pregnancy & breastfeeding – Discuss risks with your provider.
Always review your full medical history with your healthcare team before starting GLP‑1 medication.
Conclusion
“Determining the right GLP‑1 dosage doesn’t have a single answer — it depends on the specific medication, your health goals, your body’s response, and guidance from a qualified healthcare professional. Standard protocols typically start at a low dosage and increase gradually to balance effectiveness and tolerability. Always use GLP‑1 medications under medical supervision, monitor for side effects, and follow up regularly to ensure the dosage is safe and appropriate for you.
In summary, finding the optimal GLP‑1 dosage requires a personalized approach. Starting with a low dosage and titrating gradually helps maximize benefits while minimizing side effects. Your medication type, goals, and individual response all influence the correct dosage. Regular monitoring of blood sugar, weight, and overall well-being ensures the therapy remains safe and effective.
GLP‑1 medications can be a powerful tool for managing type 2 diabetes, supporting weight loss, and improving metabolic health, but they work best when combined with healthy lifestyle habits. By following medical guidance and being patient with the titration process, you can achieve positive outcomes and maintain long-term wellness while staying on the right dosage plan.
Frequently Asked Questions (FAQs)
1. Is there a universal dose for all GLP‑1 drugs?
No. Each medication (semaglutide, liraglutide, tirzepatide, etc.) has its own dosing schedule.
2. Can you take GLP‑1 without a doctor’s prescription?
No — these are prescription medications and should not be taken without professional supervision.
3. Can you adjust the dose yourself?
Self‑adjustment is not recommended. Always consult your healthcare provider.
4. How soon will I feel the effects?
Some people notice appetite changes within weeks; full therapeutic effects often take longer, especially with weight loss protocols.
5. What happens if I miss a dose?
Follow your prescriber’s instructions. For weekly meds, if a dose is missed by a few days, providers may advise taking it as soon as possible.
6. Are higher doses more effective?
Not necessarily. More isn’t always better — higher doses can increase side effects without added benefits for some users.
7. Can children take GLP‑1 medications?
Some are approved for adolescents in specific cases, but dosing and safety vary and require pediatric specialist guidance.
8. Does weight or height affect the dose?
Often, prescriptions are individualized, but dosing starts from standardized guidelines rather than strict height/weight calculations.
9. Can I switch between different GLP‑1 drugs?
Yes, but transitions should be handled by a clinician to avoid gaps or overlaps in therapy.
